
In diagnostic bronchoscopy, bronchoscopists have long faced the formidable challenge of obtaining an adequate amount of tissue from suspicious lung lesions to arrive at a definitive diagnosis despite not being able to visualize exact lesion location during the procedure. Lung cancer is the 2nd most common cancer in the world with an estimated 2.2 million new cases each year. Due to the low five-year survival rate of less than 20%, lung cancer is the leading cause of cancer death worldwide, resulting in 1.8 million deaths annually. A major contributor to the low survival rate is that only 16% of lung cancer patients are diagnosed at an early stage where the five-year survival rate stands at a promising 56%. Regrettably, most lung cancer patients are diagnosed at later stages where survivability plunges to a mere 5% and more than half of people with lung cancer die within one year of being diagnosed.1
The advent of real-time, intraoperative imaging technologies like LungVisionTM potentially changes this calculus by enabling bronchoscopists to intraprocedurally visualize and thus more confidently pursue biopsies of sub-centimeter lesions they might otherwise not attempt to diagnose. If the diagnosis is indeed cancer, it is likely at an earlier stage where timely treatment can significantly enhance survivability of these individuals.
(Source: Lung Cancer Facts 2023)2
Lung Cancer Five-Year Survival Rate
Lung cancer stands out with one of the most dismal five-year survival rates, primarily attributed to its frequently late-stage diagnosis. Globally, the average 5-year survival rate is an alarmingly low 18%.1,2
Within the United States, for example, 8 million individuals fall into the high-risk category for developing lung cancer. However, until recently, clear and robust screening guidelines from the US Preventive Services Task Force (USPSTF) were scarce. The lack of guidance, coupled with limited public awareness and other contributing factors, has resulted in only 5.8% of individuals recommended for lung cancer screening having undergone screening, lagging far behind the screening rates observed for other types of cancer. Notably, if only half of these high-risk individuals were to undergo screening, more than 12,000 American lung cancer deaths could potentially be averted.1
The timely detection of lung cancer at an earlier stage plays a vital role in enhancing treatment success and, ultimately, preserving lives. Research findings from the National Lung Screening Trial (NLST) conducted in 2011 have unequivocally demonstrated the efficacy of regular lung cancer screenings in reducing mortality rates by 20 percent. This significant finding has been further substantiated by subsequent European trials underscoring the value of early detection.5 Likewise, it comes as no surprise that Japan, which has the highest age-standardized five-year net survival for lung cancer patients at 32.9%, has a national recommendation of an annual chest X-ray for people aged 40 and over and sputum cytology for smokers aged 50 and over who have smoked more than 600 cigarettes over their lifetime, possibly leading to earlier detection relative to other nations.7 In light of this mounting clinical evidence, the US Preventive Services Task Force responded in 2021 by releasing a new guideline that recommends annual low-dose CT screening for individuals aged 50 to 80 with a history of smoking.6
The LungVisionTM Solution for Earlier, Definitive Diagnosis
The LungVisionTM system uses artificial intelligence (AI) to transform X-ray images from any C-arm into real-time, intraoperative CT scans. LungVisionTM enables bronchoscopists to see the lesion and lesion location during diagnostic bronchoscopy to aid navigation to the lesion and provide visual confirmation that they are taking biopsies from within the lesion. This novel approach enhances the likelihood of diagnosing lung cancer patients when lesions are smaller and more likely to be at an earlier stage when there are more treatment options and survival rates are higher.
In 2021, the University of Chicago Medical Center conducted a study where 45 patients underwent diagnostic bronchoscopy utilizing the LungVisionTM AI-driven, intraoperative CT imaging platform in conjunction with an Ethicon Monarch robotic bronchoscopy platform. The use of LungVisionTM real-time intraoperative CT imaging enabled the bronchoscopists to achieve a diagnostic yield of 91% in those 45 patients.8 Without intraoperative imaging, the lung cancer diagnostic success rate of clinicians performing transbronchial biopsies typically does not exceed 70%.9
LungVisionTM Real-Time Imaging: Transforming Early Detection for Patients
Generally speaking, the size of lung nodules serves as a valuable indicator of tumor progression, with smaller nodules often associated with newer, earlier-stage tumors and larger nodules often correlating to later-stage tumors with a potentially heightened risk of metastasis to other regions of the lung or to other organs.10 As a result, the detection and identification of lesions in their nascent stages assume paramount importance.
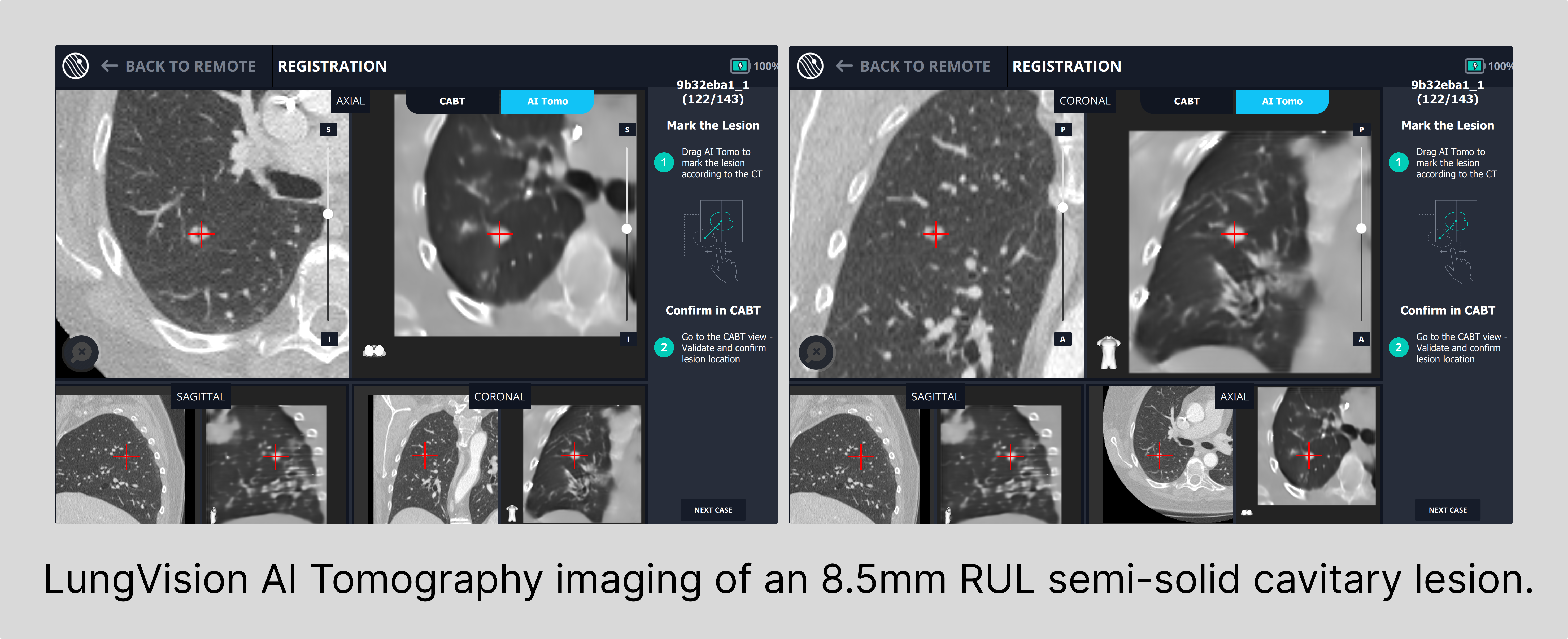
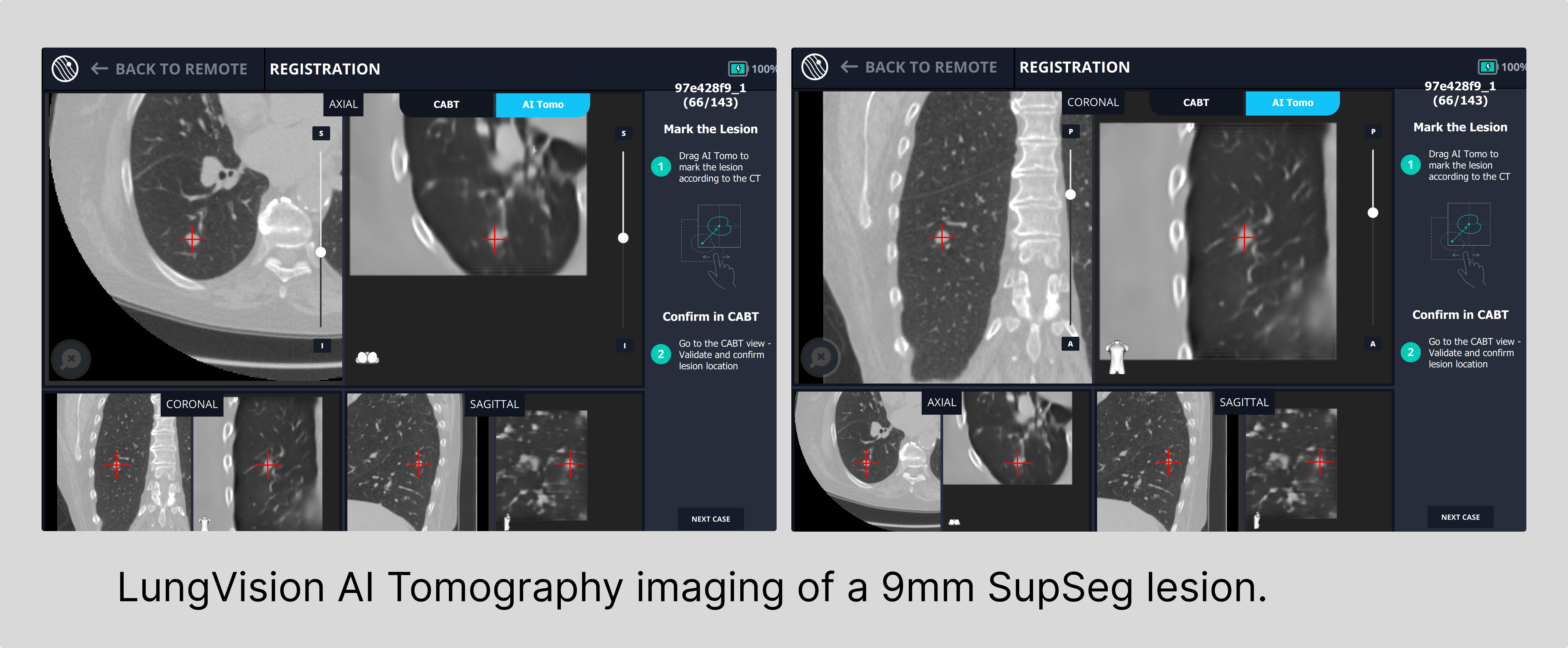
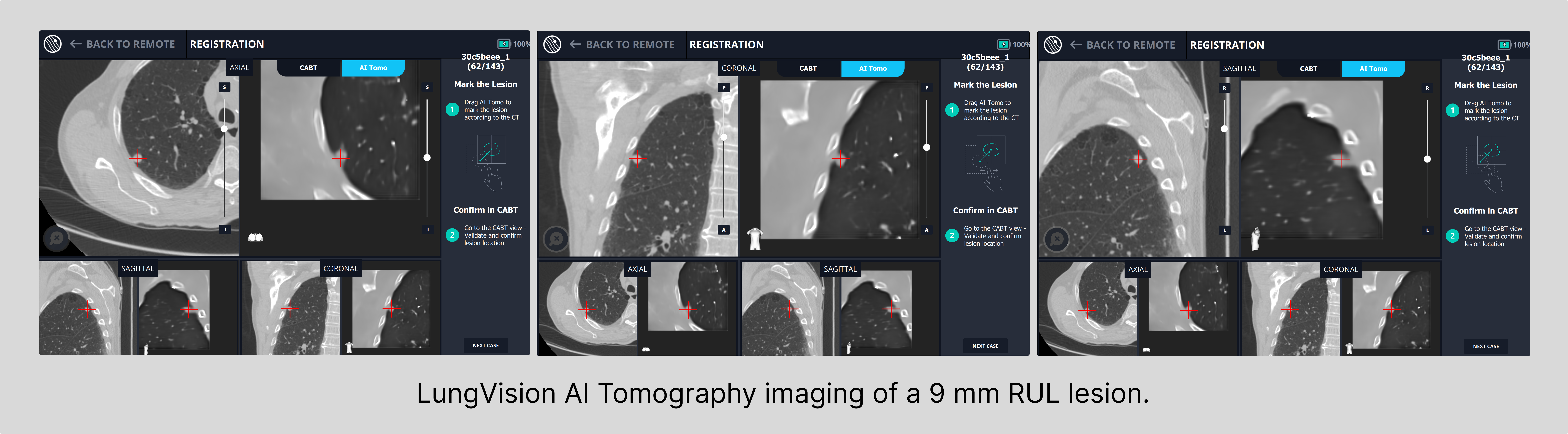
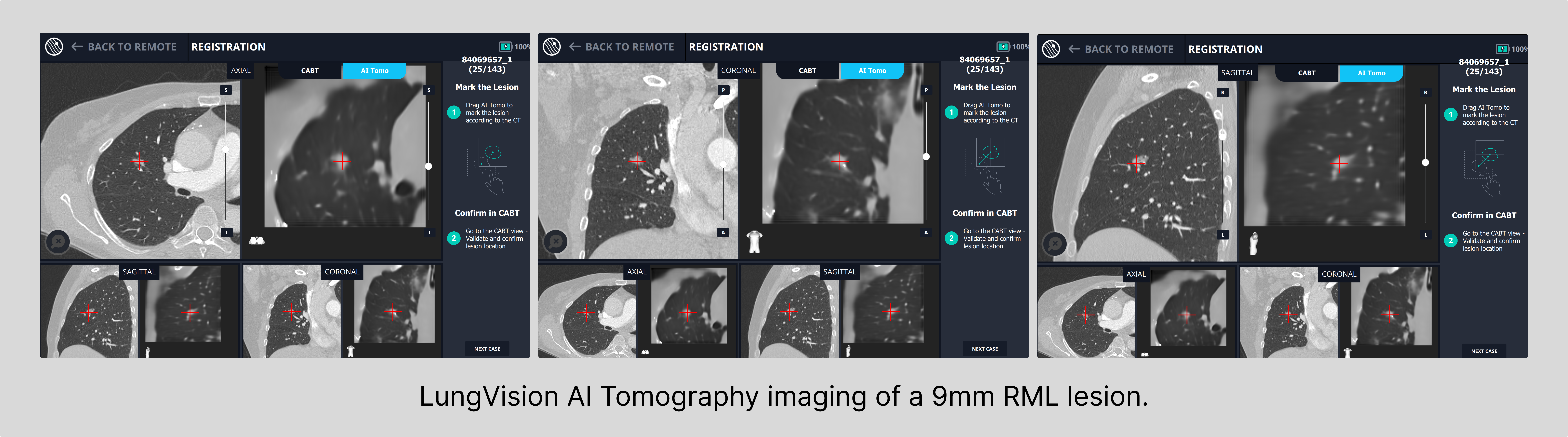
Democratizing Access to Innovative Medical Technology
Body Vision Medical strives to save lives through the democratization of innovative medical technology and the development of LungVisionTM in the pulmonary space is keeping with that ethos. Other medical technologies have been developed in an attempt to address the issue of low diagnostic yield, but most such as robotic bronchoscopy platforms and cone-beam CT (CBCT) are far too costly to be viable outside of major academic centers and metropolitan hospitals in the United States and have even lower viability outside the US. LungVisionTM seamlessly integrates into the existing procedural workflow, leverages existing equipment the hospital already has in order to reduce the cost of implementation, and, despite being an all-in-one solution for navigation and real-time imaging, is a fraction of the cost of electromagnetic navigation (EMN), robotics, or CBCT. This approach provides the intraoperative imaging necessary to achieve superior clinical results at a significantly reduced cost, making it accessible to rural and community hospitals, and more importantly, the lung patients they serve, globally.
The implementation of LungVision's real-time intraoperative imaging during diagnostic bronchoscopy empowers bronchoscopists to visualize sub-centimeter lesions intraprocedurally, accurately navigate to the lesions, and biopsy from those lesions with precision. This innovation in real-time image guidance facilitates the earlier diagnosis of a greater number of lung patients, enabling prompt treatment and potentially expediting the return to their normal daily lives.
Sources
1. Association, A. L. (n.d.). Lung cancer fact sheet. American Lung Association. https://www.lung.org/lung-health-diseases/lung-disease-lookup/lung-cancer/resource-library/lung-cancer-fact-sheet#:~:text=The%20lung%20cancer%20five%2Dyear,and%20prostate%20(98.2%20percent).&text=The%20five%2Dyear%20survival%20rate,localized%20(within%20the%20lungs
2. Lung cancer facts 2023. Lung Cancer Research Foundation. (2023, January 17). https://www.lungcancerresearchfoundation.org/lung-cancer-facts/#sources1
3. Cancer of the lung and bronchus - cancer stat facts. SEER. (n.d.). https://seer.cancer.gov/statfacts/html/lungb.html
4. Lung cancer fact sheet, 2021. (n.d.). https://member.thoracic.org/about/global-public-health/firs/resources/world-lung-cancer-day-fact-sheet-2021.pdf
5. Reduced lung-cancer mortality with low-dose computed tomographic screening. AU National Lung Screening Trial Research Team, Aberle DR, Adams AM, Berg CD, Black WC, Clapp JD, Fagerstrom RM, Gareen IF, Gatsonis C, Marcus PM, Sicks JD SO N Engl J Med. 2011;365(5):395.
6. US Preventative Services Task Force Members. (2021, March 9). Screening for Lung Cancer US Preventive Services Task Force Recommendation Statement. Recommendation: Lung Cancer: Screening | United States Preventive Services Taskforce. Retrieved November 3, 2021, from https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/lung-cancer-screening#fullrecommendationstart.
7. Incidence, survival and mortality for lung cancer. Health at a Glance: Asia/Pacific 2020 : Measuring Progress Towards Universal Health Coverage | OECD iLibrary. (n.d.). https://www.oecd-ilibrary.org/sites/19cbcb14-en/index.html?itemId=%2Fcontent%2Fcomponent%2F19cbcb14-en
8. Hedstrom G, Wagh A. Combining Real-Time 3-D Imaging and Augmented Fluoroscopy with Robotic Bronchoscopy for the Diagnosis of Peripheral Lung Nodules. Chest, Volume 162, Issue 4, Supplement, 2022, Page A2082.
9. Mehta AC, Hood KL, Schwarz Y, Solomon SB. The Evolutional History of Electromagnetic Navigation Bronchoscopy: State of the Art. Chest. 2018 Oct;154(4):935-947.
10. Shan, Q., Fan, Y., Guo, J., Han, X., Wang, H., & Wang, Z. (2019, October 10). Relationship between tumor size and metastatic site in patients with stage IV non-small cell lung cancer: A large seer-based study. PeerJ. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6790223/#:~:text=For%20brain%20or%20lung%20metastasis,of%20brain%20or%20lung%20metastasis